ARTICLES
Is tax funding of health care more likely to be regressive than systems based on social insurance in low- and middle-income countries?
¿Es posible que la financiación tributaria de la salud sea más regresiva que los sistemas basados en el aseguramiento social en países de ingreso bajo y medio?
Est-il possible que le financement des systèmes de santé par des impôts soit plus régressif que les systèmes fondés sur l'assurance sociale dans les pays à revenu faible et moyen?
Aurelio Mejía Mejía*
* Grupo de Economía de la Salud, Facultad de Ciencias Económicas, Universidad de Antioquia. Address: Calle 67 No. 53 – 108, Bloque 13, Medellín, Colombia. E-mail: [email protected].
The author thanks two anonymous reviewers who commented on an earlier version of this paper. All errors and omissions are the sole responsibility of the author.
-Introduction. -I. Measurement of health financing progressivity. -II. What does the empirical evidence suggest? –Conclusions. –References.
Primera versión recibida el 16 de septiembre de 2012; versión final aceptada el 22 de marzo de 2013
ABSTRACT
One of the main functions of health care systems is to collect enough revenue to finance health expenditures. This revenue can be obtained through different sources (taxes, social insurance contributions, out-of-pocket payments, donations), each of which has different implications in terms of equity. The equity implications of the different forms of revenue collection are an important component of health systems performance evaluation. The international evidence suggests that tax funded systems seem to be a more progressive health care financing mechanism than systems based on social insurance in low- and middle-income countries. However, progressivity results are sensitive to the choice of ability to pay measures and, therefore, policy makers must be aware of this fact when interpreting results of studies on health care financing.
Key words: health systems financing, progressivity, equity.
JEL classification: I11, I14.RESUMEN
Una de las funciones principales de los sistemas de salud es recaudar recursos suficientes para financiar el gasto en salud. Estos recursos provienen de diversas fuentes (impuestos, donaciones, contribuciones a la seguridad social, gasto de bolsillo), las cuales pueden tener diferentes implicaciones en términos de equidad, componente clave en la evaluación del desempeño de los sistemas sanitarios. La evidencia internacional sugiere que en los países de ingresos bajos y medios los sistemas que recaudan los ingresos fundamentalmente vía impuestos tienden a ser más progresivos que los sistemas basados en aseguramiento. Sin embargo, este resultado depende de la medida de capacidad de pago elegida y, por lo tanto, los responsables de tomar decisiones deben tener en cuenta este hecho al interpretar los resultados de los estudios sobre la progresividad en el financiamiento de los sistemas de salud.
Palabras clave: financiamiento de sistemas de salud, progresividad, equidad.
Clasificación JEL: I11, I14.RÉSUMÉ
L'une des principales fonctions des systèmes de santé est celui de collecter des fonds suffisamment pour financer les dépenses de santé. Ces fonds ont une diversité des sources (taxes, contributions de sécurité sociale, dépenses de poche, donations), lesquels peuvent avoir des implications en termes d'équité, ce qui constitue un élément clé dans l'évaluation de la performance des systèmes de santé. L'expérience internationale montre que les pays à faible revenu et les pays à revenu moyens qui ont des systèmes de santé financés par les impôts, sont plus progressistes par rapport aux systèmes de santé financés par l'assurance sociale. Toutefois, ce résultat dépend de la mesure choisie entant que capacité de paiement. Par conséquent, les responsables de la politique de santé doivent avoir très présent ce fait lors de leur interprétation des résultats des études concernant la progressivité dans le financement des systèmes de santé.
Mots-clés: financement des systèmes de santé, progressivité, équité.
Classification JEL: I11, I14.
INTRODUCTION
One of the main functions of health care systems is to collect enough revenue to finance health expenditures. This revenue can be obtained through different sources: general taxation (including direct and indirect taxes), social insurance contributions, out-of-pocket payments and even grants or donations (Mossialos & Dixon, 2002). Given that societies usually prefer to provide services according to some measure of need, and at the same time it is argued that ability to pay should determine individuals' contribution to health care financing, equity implications of the different forms of revenue collection are an important component of health systems performance evaluation. One explicit concern is the extent to which health care financing promotes vertical equity, and particularly how ''payments for health care rise or fall as a proportion of a person's income'' (Wagstaff & Van Doorslaer, 2000, pp. 1819). Health care financing can be either progressive, if payments rise as income increases, regressive, if the opposite happens, or proportional, if the proportion of income devoted to health care payments is the same regardless of an individual's income.
An increasing awareness of the impoverishing effects of out-of-pocket payments in low- and middle-income countries (LMICs) has motivated reforms that favour pre-payment mechanisms for health care financing, particularly general taxation and social insurance (McIntyre, 2007; Wagstaff, 2007). Because of the structure of taxation, it might be argued that tax funding of health care is likely to be more regressive than systems based on social insurance in LMICs. However, evidence must be carefully analysed before any policy is implemented. Hence the purpose of this essay is to describe how this argument can be assessed and to discuss how empirical evidence can be used to illuminate this issue.
I. Measurement of health care financing progressivity
The most common way to assess the progressivity of health systems financing is the Kakwani's progressivity index, which measures the extent to which a source of finance departs from proportionality (Wagstaff & van Doorslaer, 2000; Kakwani, 1977). Even though this is not the only index available to analyze progressivity of health care financing, this article will focus on the Kakwani index given its widespread application in empirical studies. Another index, proposed by the World Health Organization, is the index of fairness of financial contribution, but its ability to discriminate between regressive and progressive systems has been disputed (Wagstaff, 2002).
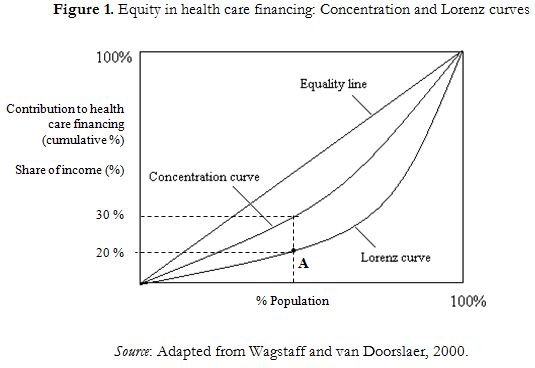
The Kakwani index can be calculated using the information in Figure 1. The Lorenz curve represents income inequality: it orders the population according to the share of income. If income is distributed equally, the Lorenz curve would overlap the equality line; but if income is distributed in such a way that the poorest 20% of population has an income share of less than 20% and so on, then it would lie below the equality line, as in Figure 1. To measure income inequality, the Gini coefficient can be calculated as twice the area between the equality line and the Lorenz curve. On the other hand, the concentration curve ranks individuals according to income and plots them against the cumulative proportion of the contribution to health care financing. It is also possible to calculate the concentration index as twice the area between the equality line and the concentration curve.
Figure 1 illustrates the case in which the poorer households contribute disproportionately more than the rich to health care financing. For example, consider point A, which approximately corresponds to the 50% of population. In this case, the poorest half of the population receives lets say only 20% of income, but they contribute to 30% of total health care financing.
The Kakwani index (K) is based on the difference between the Lorenz and concentration curves and can be calculated as follows:
K = C – G (1)
where C corresponds to the concentration index of the contributions to healthcare financing and G to the Gini coefficient for income (before contributions). The Kakwani index is bounded by –2 and 1. Negative values indicate that the concentration curve lies above the Lorenz curve and therefore the financing system can be regarded as regressive, as is the case illustrated in Figure 1. In a proportional system, both curves overlap and the index is equal to zero. Finally, positive values correspond to progressive systems (the concentration curve lies below the Lorenz curve). One attractive property of the Kakwani index is that if revenue is collected from different sources, overall progressivity can be calculated as the weighted average of the Kakwani index for the different sources, using the proportion of each source to total revenue as weights (O'Donnell et al., 2008a).
It is important to emphasize that the index is not a replacement for the graphical analysis (O'Donnell et al., 2008a). For example, a Kakwani index of zero may be a consequence of a system that is progressive for lower income persons but regressive as income increases (the Lorenz and concentration curves would cross), or the other way around. Evidently, each situation requires different policy responses: while the first case may be considered acceptable (policymakers may be willing to accept a system in which the poorest groups contribute proportionately less and richer groups contribute proportionately more), the reverse situation could be judged as socially unacceptable. If the Kakwani index is equal to zero because Lorenz and concentration curve cross, health policy that only relies on the index number could exacerbate the effect of income inequality.
With the previous results, it is possible to assess the progressivity of tax funded health systems: they will be more or less progressive according to general tax progressivity, which in turn depends on the burden of indirect and direct taxes. Direct taxes, like income, vehicle or profit taxes, are generally more progressive (Savedoff, 2004), while indirect taxes, like the value added tax, tend to be more regressive because they are levied on consumption goods and low income households tend to expend proportionally more of their income in those taxes. On the other hand, progressivity of systems based on social health insurance depends on the way revenue is collected and the coverage of insurance, and in principle there are no theoretical reasons to believe that tax funded systems are likely to be more regressive than systems based on social insurance in LMICs. As a matter of fact, given that social insurance contributions are generally a percentage of formal worker's salaries (Savedoff, 2004) and there are contributions ceilings (Wagstaff, 2007), social insurance is potentially more regressive than a tax funded system.
II. What does the empirical evidence suggest?
In high income countries, Wagstaff et al. (1999) show that direct taxes are progressive in thirteen OECD countries, indirect taxes are regressive in all of them, and social insurance is progressive in all but two countries where high income individuals can opt out the system (Germany and Netherlands). O'Donnell et al. (2008b) also found that in Japan, South Korea and Taiwan, countries with systems based on social insurance, health care financing is slightly regressive.
Regarding LMICs, O'Donnell et al. (2008b) found Kakwani indexes close to one for direct tax payments in countries like Bangladesh, the Philippines, Sri Lanka and Thailand, which means that these taxes are paid mainly by the richer individuals. Similarly, the index for indirect taxes is also positive, which means that they are also a progressive way to finance health care. This result is a consequence of the fact that in these countries taxes are normally applied to luxury goods and basic consumption goods are exempt. Finally, the study also found a positive index for social insurance payments. However, the reason behind this finding is that coverage is generally restricted to formal working groups, and such a situation is far from an equitable outcome (Rannan-Eliya & Somanathan, 2006).
In Palestine, governmental health insurance appears slightly progressive; but this effect is offset by out-of-pocket payments (approximately 40% of total health expenditures), resulting in an overall Kakwani index of –0.0677 for the West Bank and –0.0473 for the Gaza Strip in 2004 (Abu-Zaineh et al., 2008). Thus, progressivity in insurance could not compensate for the negative effect of out-of-pocket payments given their dominance in the Palestinian financing mix. In Africa, Cissé et al. (2007) analyze progressivity in health care finance in four West African capital cities: Abidjan (Ivory Coast), Bamako (Mali), Conakry (Guinea) and Dakar (Senegal). Given the absence of public or private health insurance, out-of-pocket payments constitute a significant proportion of total revenue and, as a consequence, the health care financing is regressive in all four cities: The Kakwani index ranges from –0.08 in Dakar to –0.52 in Conakry.
Hajizadeh and Connelly (2009) analyse health care financing in Iran, where government expenditure accounts for 50% of health care financing (30% of resources correspond to taxation and 70% to natural resource sales) and private expenditure for the remaining 50% (mainly private insurance and co-payments). The Kakwani index for total private health expenditure between 1995 and 2005 is always positive and relatively stable around 0.1, if household expenditure is used as the ability to pay variable. However, if household income is used instead of expenditures, results point towards a mildly regressive system: The Kakwani index is between –0.01 and –0.17, except in 2004/2005 when the index is positive (0.00599). Following the authors, who prefer expenditure measures as these show less variance over time and are probably less underestimated than income (O'Donnell et al., 2008a), consumer co-payments are progressive in both urban and rural areas of Iran, while social insurance payments are generally progressive in rural areas but regressive in urban areas.
Finally, in Colombia, social health insurance was introduced in 1993 to offer universal coverage to the population and to reduce out-of-pocket payments, which are widely regarded as one of the most regressive financing mechanisms (McIntyre, 2007). To analyse the impact of the reform, Castaño et al. (2002) calculated the Kakwani index for out-of-pocket payments before the reform and one and four years after its implementation. Despite some methodological shortcomings, they found a movement towards progressivity when using expenditures as the indicator of ability to pay. However, similarly to the Iranian findings, results indicate a regressive system if income is used as the ability to pay indicator. On the other hand, in Brazil, a study by Ugá and Santos (2007) showed that the financing system (where 44% of total expenditure is tax funded) is slightly regressive: While direct taxes were progressive (basically income and vehicle taxes), this effect was offset by the regressive effect of indirect taxes and out-of-pocket payments. The authors do not use the Kakwani index, but instead they calculate the contribution of each decile to health financing by source of funding.
Conclusions
As the evidence shows, social insurance contributions and taxes are two different ways to finance health systems that entail different implications regarding the progressivity of the system in LMICs. The Kakwani progressivity index and concentration curves can help policy makers to analyse the extent to which contributions fall or rise as income increases, and therefore they are valuable tools in the design and evaluation of health reforms in LMICs.
In the case of tax funded systems, the evidence suggests that direct and even indirect taxes can be progressive sources of financing in LMICs provided that indirect taxes are applied only to luxury goods and basic consumption goods are exempt. For systems based on social insurance, the evidence is less conclusive. Even when the Kakwani index is positive in some LMICs, this does not necessarily mean that social insurance payments are a progressive source of health care financing. On the contrary, it might reflect an access problem: richer groups pay proportionately more than poorer households but enjoy higher quality and access to health care.
The findings in various LMICs indicate that tax funded systems seem to be a more progressive health care financing mechanism and the claim that they are likely to be more regressive than systems based on social insurance is not justified. However, as the results for Colombia and Iran demonstrate, it is important to note that progressivity results are sensitive to the choice of the ability to pay measure and, therefore, policy makers must be aware of this fact when interpreting the results of studies on health care financing.
This paper presented a brief introduction to the measurement of equity implications of different forms of health care funding and a review of some empirical findings. Future studies could do a more comprehensive empirical evaluation that might yield more definitive findings and a stronger guide for policy makers who are considering alternative funding arrangements for health care systems.
References
Abu-zaineh, Mohammad; Mataria, Awad; Luchini, Stéphane & Moatti, Jean Paul (2008). ''Equity in health care financing in Palestine: The value-added of the disaggregate approach'', Social Science & Medicine, Vol. 66, Issue 11, pp. 2308-2320.
Castaño, Ramón; Arvelaez, José; Giedion, Úrsula & Morales, Luis (2002). ''Equitable financing, out-of-pocket payments and the role of health care reform in Colombia'', Health Policy and Planning, vol. 17, Suppl. 1, pp. 5-11.
Cissé, Boubou; Luchini, Stéphane & Moatti, Jean Paul (2007). ''Progressivity and horizontal equity in health care finance and delivery: What about Africa?'' Health Policy, Vol. 80, Issue 1, pp. 51-68.
Hajizadeh, Mohammad & Connelly, Luke (2009). ''Equity of health care financing in Iran''. ACERH Working Paper, Issue 5, available at http://mpra.ub.uni-muenchen.de/14672/1/ACERH_WP5_unsecured.pdf (31 March 2009).
Kakwani, Nanak C. (1977). ''Measurement of Progressivity: An International Comparison'', The Economic Journal, Vol. 87, No. 345, pp. 71-80.
McIntyre, Diane (2007). Learning from experience: health care financing in low- and middle-income countries, Geneva, Global Forum for Health Research.
Mossialos, Elias & Dixon, Anna (2002). ''Funding health care: An introduction''. In: Mossialos, Elias; Dixon, Anna; Figueras, Josep & Kutzin, Joe (Eds.). Funding Health Care. Options for Europe (pp.1-30). Buckingham, Open University Press.
O'donnell, Owen; van Doorslaer, Eddy; Wagstaff, Adam & Lindelow, Magnus (2008a). Analyzing Health Equity Using Household Survey Data, Washington, The World Bank.
O'donnell, Owen; van Doorslaer, Eddy; Rannan-eliya, Ravi; Somanathan, Aparnaa; Adhikari, Shiva Raj; Akkazieva, Baktygul... Yuxin, Zao (2008b). ''Who pays for health care in Asia?'' Journal of Health Economics, Vol. 27, Issue 2, pp. 460-475.
Rannan-eliya, Ravindra & Somanathan, Aparnaa (2006). ''Equity in health and health care systems in Asia''. In: Jones, Andrew (Ed.). The Elgar Companion to Health Economics (pp. 205-218). Cheltenham, UK & Northampton, USA, Edward Elgar.
Savedoff, William (2004). ''Tax-Based Financing for Health Systems: Options and Experiences''. World Health Organization, available at: http://www.who.int/health_financing/documents/dp_e_04_4-taxed_based_financing.pdf (31 March 2009).
Ugá, M., and Santos, I. (2007). ''An analysis of equity in Brazilian health system financing''. Health Affairs (Millwood), vol. 26, issue 4, pp. 1017-1028.
Wagstaff, Adam (2002). ''Reflections on and alternatives to WHO's fairness of financial contribution index'', Health Economics, Vol. 11, Issue 2, pp. 103-15.
Wagstaff, Adam (2007). ''Social Health Insurance Reexamined.'' World Bank Policy Research Working Paper, Issue4111, available at: http://www-wds.worldbank.org/external/default/WDSContentServer/IW3P/IB/2007/01/09/000016406_20070109161148/Rendered/PDF/wps4111.pdf (31 March 2009).
Wagstaff Adam, van Doorslaer, Eddy, VAN DER BURG H, et al. (1999). Equity in the finance of health care: some further international comparisons. Journal of Health Economics, Vol. 18, No. 3, pp. 263-90.
Wagstaff, Adam and van Doorslaer, Eddy (2000). ''Equity in Health Care Finance and Delivery''. In: Culyer, Anthony and Newhouse, Joseph (Eds.). Handbook of Health Economics, (Vol. 2) (pp. 1803-1862). Amsterdam, Elsevier Science B. V.