Esclerosis lateral amiotrófica: actualización
DOI:
https://doi.org/10.17533/udea.iatreia.v29n2a08Palabras clave:
diagnóstico, enfermedad de la neurona motora, epidemiología, esclerosis amiotrófica lateral, signos y síntomas, terapéuticaResumen
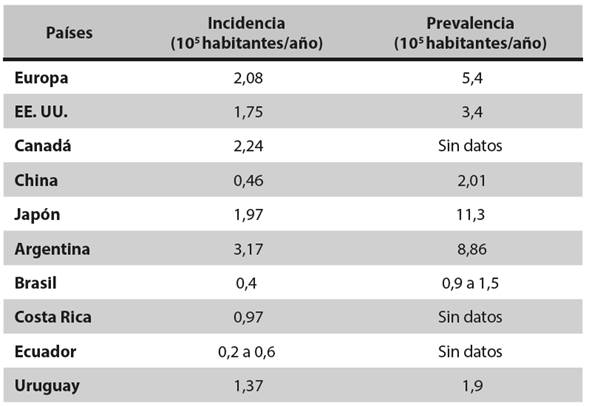
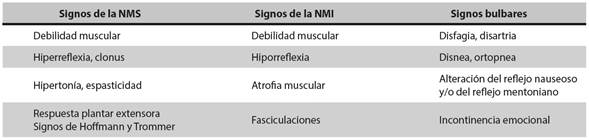
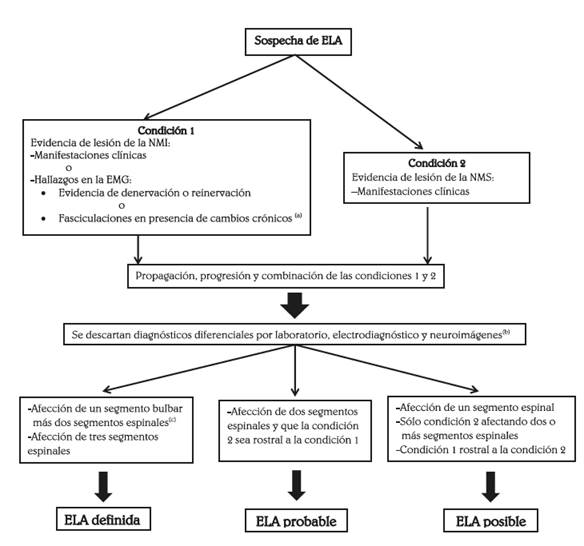
La esclerosis lateral amiotrófica es una enfermedad neurodegenerativa que tiene consecuencias devastadoras para el paciente y su familia. Aún no existe claridad sobre su etiología, cerca del 10% de los pacientes tienen patrón hereditario. La prevalencia mundial varía entre 2 y 11 casos por 100.000 habitantes; el rango de edad de presentación es de 58 a 63 años para los casos esporádicos, y de 47 a 52 años para los familiares, con una ligera predilección por el sexo masculino. Las manifestaciones clínicas incluyen signos de daño de las neuronas motoras superior e inferior tanto en las extremidades como en la musculatura bulbar, y en algunos pacientes hay deterioro cognitivo frontotemporal. El diagnóstico continúa siendo fundamentalmente clínico, apoyado por estudios neurofisiológicos; de estos, la electromiografía de aguja ha sido el más útil para el diagnóstico temprano. No existe tratamiento curativo y solo un medicamento, el riluzol, ha demostrado efectividad para retrasar el uso de ventilación mecánica y prolongar levemente la supervivencia. Por tanto, el tratamiento de estos pacientes se basa en medidas de soporte, especialmente en los aspectos de nutrición y ventilación, además de controlar los síntomas motores y no motores de la enfermedad.
Descargas
Citas
(1.) Hardiman O, van den Berg LH, Kiernan MC. Clinical diagnosis and management of amyotrophic lateral sclerosis. Nat Rev Neurol. 2011 Oct;7(11):639-49. DOI 10.1038/nrneurol.2011.153.
(2.) Andersen PM, Al-Chalabi A. Clinical genetics of amyotrophic lateral sclerosis: what do we really know? Nat Rev Neurol. 2011 Oct;7(11):603-15. DOI 10.1038/nrneurol.2011.150.
(3.) Ravits JM, La Spada AR. ALS motor phenotype heterogeneity, focality, and spread: deconstructing motor neuron degeneration. Neurology. 2009 Sep;73(10):805-11. DOI 10.1212/WNL.0b013e3181b6bbbd.
(4.) D’Amico E, Factor-Litvak P, Santella RM, Mitsumoto H. Clinical perspective on oxidative stress in sporadic amyotrophic lateral sclerosis. Free Radic Biol Med. 2013 Dec;65:509-27. DOI 10.1016/j.freeradbiomed.2013.06.029.
(5.) Spreux-Varoquaux O, Bensimon G, Lacomblez L, Salachas F, Pradat PF, Le Forestier N, et al. Glutamate levels in cerebrospinal fluid in amyotrophic lateral sclerosis: a reappraisal using a new HPLC method with coulometric detection in a large cohort of patients. J Neurol Sci. 2002 Jan;193(2):73-8.
(6.) Menzies FM, Ince PG, Shaw PJ. Mitochondrial involvement in amyotrophic lateral sclerosis. Neurochem Int. 2002 May;40(6):543-51.
(7.) Tomkins J, Usher P, Slade JY, Ince PG, Curtis A, Bushby K, et al. Novel insertion in the KSP region of the neurofilament heavy gene in amyotrophic lateral sclerosis (ALS). Neuroreport. 1998 Dec;9(17):3967-70.
(8.) Julien JP. ALS: astrocytes move in as deadly neighbors. Nat Neurosci. 2007 May;10(5):535-7.
(9.) Sathasivam S, Ince PG, Shaw PJ. Apoptosis in amyotrophic lateral sclerosis: a review of the evidence. Neuropathol Appl Neurobiol. 2001 Aug;27(4):257-74.
(10.) Shaw PJ. Molecular and cellular pathways of neurodegeneration in motor neurone disease. J Neurol Neurosurg Psychiatry. 2005 Aug;76(8):1046-57.
(11.) Vinsant S, Mansfield C, Jimenez-Moreno R, Del Gaizo Moore V, Yoshikawa M, Hampton TG, et al. Characterization of early pathogenesis in the SOD1(G93A) mouse model of ALS: part II, results and discussion. Brain Behav. 2013 Jul;3(4):431-57. DOI 10.1002/brb3.142.
(12.) de Jong SW, Huisman MH, Sutedja NA, van der Kooi AJ, de Visser M, Schelhaas HJ, et al. Smoking, alcohol consumption, and the risk of amyotrophic lateral sclerosis: a population-based study. Am J Epidemiol. 2012 Aug;176(3):233-9. DOI 10.1093/aje/kws015.
(13.) Sutedja NA, Veldink JH, Fischer K, Kromhout H, Heederik D, Huisman MH, et al. Exposure to chemicals and metals and risk of amyotrophic lateral sclerosis: a systematic review. Amyotroph Lateral Scler. 2009 Oct-Dec;10(5-6):302-9. DOI 10.3109/17482960802455416.
(14.) Chiò A, Benzi G, Dossena M, Mutani R, Mora G. Severely increased risk of amyotrophic lateral sclerosis among Italian professional football players. Brain. 2005 Mar;128(Pt 3):472-6.
(15.) Chiò A, Calvo A, Dossena M, Ghiglione P, Mutani R, Mora G. ALS in Italian professional soccer players: the risk is still present and could be soccer-specific. Amyotroph Lateral Scler. 2009 Aug;10(4):205-9. DOI 10.1080/17482960902721634.
(16.) Armon C, Nelson LM. Is head trauma a risk factor for amyotrophic lateral sclerosis? An evidence based review. Amyotroph Lateral Scler. 2012 Jun;13(4):351-6. DOI 10.3109/17482968.2012.660954.
(17.) Kihira T, Okamoto K, Yoshida S, Kondo T, Iwai K, Wada S, et al. Environmental characteristics and oxidative stress of inhabitants and patients with amyotrophic lateral sclerosis in a high-incidence area on the Kii Peninsula, Japan. Intern Med. 2013;52(13):1479-86.
(18.) Caller TA, Chipman JW, Field NC, Stommel EW. Spatial analysis of amyotrophic lateral sclerosis in Northern New England, USA, 1997-2009. Muscle Nerve. 2013 Aug;48(2):235-41. DOI 10.1002/mus.23761.
(19.) Siddique T, Figlewicz DA, Pericak-Vance MA, Haines JL, Rouleau G, Jeffers AJ, et al. Linkage of a gene causing familial amyotrophic lateral sclerosis to chromosome 21 and evidence of genetic-locus heterogeneity. N Engl J Med. 1991 May;324(20):1381-4. Erratum in: N Engl J Med. 1991 Jul;325(1):71.
(20.) Rosen DR, Siddique T, Patterson D, Figlewicz DA, Sapp P, Hentati A, et al. Mutations in Cu/Zn superoxide dismutase gene are associated with familial amyotrophic lateral sclerosis. Nature. 1993 Mar;362(6415):59-62. Erratum in: Nature. 1993 Jul;364(6435):362.
(21.) Arai T, Hasegawa M, Akiyama H, Ikeda K, Nonaka T, Mori H, et al. TDP-43 is a component of ubiquitin-positive tau-negative inclusions in frontotemporal lobar degeneration and amyotrophic lateral sclerosis. Biochem Biophys Res Commun. 2006 Dec;351(3):602-11.
(22.) Kwiatkowski TJ Jr, Bosco DA, Leclerc AL, Tamrazian E, Vanderburg CR, Russ C, et al. Mutations in the FUS/TLS gene on chromosome 16 cause familial amyotrophic lateral sclerosis. Science. 2009 Feb;323(5918):1205-8. DOI 10.1126/science.1166066.
(23.) De Jesus-Hernandez M, Mackenzie IR, Boeve BF, Boxer AL, Baker M, Rutherford NJ, et al. Expanded GGGGCC hexanucleotide repeat in noncoding region of C9ORF72 causes chromosome 9p-linked FTD and ALS. Neuron. 2011 Oct;72(2):245-56. DOI 10.1016/j.neuron.2011.09.011.
(24.) Renton AE, Majounie E, Waite A, Simón-Sánchez J, Rollinson S, Gibbs JR, et al. A hexanucleotide repeat expansion in C9ORF72 is the cause of chromosome 9p21-linked ALS-FTD. Neuron. 2011 Oct;72(2):257-68. DOI 10.1016/j.neuron.2011.09.010.
(25.) Shatunov A, Mok K, Newhouse S, Weale ME, Smith B, Vance C, et al. Chromosome 9p21 in sporadic amyotrophic lateral sclerosis in the UK and seven other countries: a genome-wide association study. Lancet Neurol. 2010 Oct;9(10):986-94. DOI 10.1016/S1474-4422(10)70197-6. Erratum in: Lancet Neurol. 2011 Mar;10(3):205.
(26.) Kiernan MC, Vucic S, Cheah BC, Turner MR, Eisen A, Hardiman O, et al. Amyotrophic lateral sclerosis. Lancet. 2011 Mar;377(9769):942-55. DOI 10.1016/S0140-6736(10)61156-7.
(27.) Chiò A, Logroscino G, Traynor BJ, Collins J, Simeone JC, Goldstein LA, et al. Global epidemiology of amyotrophic lateral sclerosis: a systematic review of the published literature. Neuroepidemiology. 2013;41(2):118-30. DOI 10.1159/000351153.
(28.) Logroscino G, Traynor BJ, Hardiman O, Chiò A, Mitchell D, Swingler RJ, et al. Incidence of amyotrophic lateral sclerosis in Europe. J Neurol Neurosurg Psychiatry. 2010 Apr;81(4):385-90. DOI 10.1136/jnnp.2009.183525.
(29.) Cronin S, Hardiman O, Traynor BJ. Ethnic variation in the incidence of ALS: a systematic review. Neurology. 2007 Mar;68(13):1002-7.
(30.) Bettini M, Vicens J, Giunta DH, Rugiero M, Cristiano E. Incidence and prevalence of amyotrophic lateral sclerosis in an HMO of Buenos Aires, Argentina. Amyotroph Lateral Scler Frontotemporal Degener. 2013 Dec;14(7-8):598-603. DOI 10.3109/21678421.2013.808225.
(31.) Dietrich-Neto F, Callegaro D, Dias-Tosta E, Silva HA, Ferraz ME, Lima JM, et al. Amyotrophic lateral sclerosis in Brazil: 1998 national survey. Arq Neuropsiquiatr. 2000 Sep;58(3A):607-15.
(32.) Rodríguez- Paniagua P, Salas- Herrera I, Cartín- Brenes M. Incidencia de esclerosis lateral amiotrófica en Costa Rica. Acta Méd Costarric. 2007 Ene-Mar;49(1):33-7.
(33.) Bucheli M, Andino A, Montalvo M, Cruz J, Atassi N, Berry J, et al. Amyotrophic lateral sclerosis: analysis of ALS cases in a predominantly admixed population of Ecuador. Amyotroph Lateral Scler Frontotemporal Degener. 2014 Mar;15(1-2):106-13. DOI 10.3109/21678421.2013.852590.
(34.) Vázquez MC, Ketzoián C, Legnani C, Rega I, Sánchez N, Perna A, et al. Incidence and prevalence of amyotrophic lateral sclerosis in Uruguay: a populationbased study. Neuroepidemiology. 2008;30(2):105-11. DOI 10.1159/000120023.
(35.) Martínez HR, Molina-López JF, Cantú-Martínez L, González-Garza MT, Moreno-Cuevas JE, Couret-Alcaraz P, et al. Survival and clinical features in Hispanic amyotrophic lateral sclerosis patients. Amyotroph Lateral Scler. 2011 May;12(3):199-205. DOI 10.3109/17482968.2010.550302.
(36.) Zaldivar T, Gutierrez J, Lara G, Carbonara M, Logroscino G, Hardiman O. Reduced frequency of ALS in an ethnically mixed population: a population-based mortality study. Neurology. 2009 May;72(19):1640-5. DOI 10.1212/WNL.0b013e3181a55f7b.
(37.) Ortiz Corredor F, Mendoza Pulido C, Peña Preciado M. Diseño de un sistema de clasificación para evaluar el grado de discapacidad de los pacientes con esclerosis lateral amiotrófica. Rev Col Med Fis Rehab. 2011;21(1):14-22.
(38.) Riku Y, Atsuta N, Yoshida M, Tatsumi S, Iwasaki Y, Mimuro M, et al. Differential motor neuron involvement in progressive muscular atrophy: a comparative study with amyotrophic lateral sclerosis. BMJ Open. 2014 May;4(5):e005213. DOI 10.1136/bmjopen-2014-005213.
(39.) Chieia MA, Oliveira AS, Silva HC, Gabbai AA. Amyotrophic lateral sclerosis: considerations on diagnostic criteria. Arq Neuropsiquiatr. 2010 Dec;68(6):837-42.
(40.) Strong MJ, Grace GM, Freedman M, Lomen-Hoerth C, Woolley S, Goldstein LH, et al. Consensus criteria for the diagnosis of frontotemporal cognitive and behavioural syndromes in amyotrophic lateral sclerosis. Amyotroph Lateral Scler. 2009 Jun;10(3):131-46. Erratum in: Amyotroph Lateral Scler. 2009 Aug;10(4):252.
(41.) Consonni M, Iannaccone S, Cerami C, Frasson P, Lacerenza M, Lunetta C, et al. The cognitive and behavioural profile of amyotrophic lateral sclerosis: application of the consensus criteria. Behav Neurol. 2013;27(2):143-53. DOI 10.3233/BEN-2012-110202.
(42.) Pringle CE, Hudson AJ, Munoz DG, Kiernan JA, Brown WF, Ebers GC. Primary lateral sclerosis. Clinical features, neuropathology and diagnostic criteria. Brain. 1992 Apr;115 ( Pt 2):495-520.
(43.) D’Amico E, Pasmantier M, Lee YW, Weimer L, Mitsumoto H. Clinical evolution of pure upper motor neuron disease/dysfunction (PUMMD). Muscle Nerve. 2013 Jan;47(1):28-32. DOI 10.1002/mus.23496. Erratum in: Muscle Nerve. 2014 Oct;50(4):619.
(44.) Kim WK, Liu X, Sandner J, Pasmantier M, Andrews J, Rowland LP, et al. Study of 962 patients indicates progressive muscular atrophy is a form of ALS. Neurology. 2009 Nov;73(20):1686-92. DOI 10.1212/WNL.0b013e3181c1dea3.
(45.) Karam C, Scelsa SN, Macgowan DJ. The clinical course of progressive bulbar palsy. Amyotroph Lateral Scler. 2010 Aug;11(4):364-8. DOI 10.3109/17482960903513159.
(46.) Costa J, Swash M, de Carvalho M. Awaji criteria for the diagnosis of amyotrophic lateral sclerosis:a systematic review. Arch Neurol. 2012 Nov;69(11):1410-6.
(47.) EFNS Task Force on Diagnosis and Management of Amyotrophic Lateral Sclerosis; Andersen PM, Abrahams S, Borasio GD, de Carvalho M, Chio A, et al. EFNS guidelines on the clinical management of amyotrophic lateral sclerosis (MALS)--revised report of an EFNS task force. Eur J Neurol. 2012 Mar;19(3):360-75. DOI 10.1111/j.1468-1331.2011.03501.x.
(48.) Alvarez-Uría Tejero MJ, Sáiz Ayala A, Fernández Rey C, Santamarta Liébana ME, Costilla García S. Diagnóstico de la esclerosis lateral amiotrófica: avances en RM. Radiologia. 2011 Mar-Apr;53(2):146-55. DOI 10.1016/j.rx.2010.10.004.
(49.) Wang S, Poptani H, Bilello M, Wu X, Woo JH, Elman LB, et al. Diffusion tensor imaging in amyotrophic lateral sclerosis: volumetric analysis of the corticospinal tract. AJNR Am J Neuroradiol. 2006 Jun-Jul;27(6):1234-8.
(50.) Chiò A, Battistini S, Calvo A, Caponnetto C, Conforti FL, Corbo M, et al. Genetic counselling in ALS: facts, uncertainties and clinical suggestions. J Neurol Neurosurg Psychiatry. 2014 May;85(5):478-85. DOI 10.1136/jnnp-2013-305546.
(51.) Brooks BR. El Escorial World Federation of Neurology criteria for the diagnosis of amyotrophic lateral sclerosis. Subcommittee on Motor Neuron Diseases/Amyotrophic Lateral Sclerosis of the World Federation of Neurology Research Group on Neuromuscular Diseases and the El Escorial “Clinical limits of amyotrophic lateral sclerosis” workshop contributors. J Neurol Sci. 1994 Jul;124 Suppl:96-107.
(52.) Brooks BR, Miller RG, Swash M, Munsat TL; World Federation of Neurology Research Group on Motor Neuron Diseases. El Escorial revisited: revised criteria for the diagnosis of amyotrophic lateral sclerosis. Amyotroph Lateral Scler Other Motor Neuron Disord. 2000 Dec;1(5):293-9.
(53.) Traynor BJ, Codd MB, Corr B, Forde C, Frost E, Hardiman OM. Clinical features of amyotrophic lateral sclerosis according to the El Escorial and Airlie House diagnostic criteria: A population-based study. Arch Neurol. 2000 Aug;57(8):1171-6.
(54.) de Carvalho M, Dengler R, Eisen A, England JD, Kaji R, Kimura J, et al. Electrodiagnostic criteria for diagnosis of ALS. Clin Neurophysiol. 2008 Mar;119(3):497-503. DOI 10.1016/j.clinph.2007.09.143.
(55.) Aggarwal S, Cudkowicz M. ALS drug development: reflections from the past and a way forward. Neurotherapeutics. 2008 Oct;5(4):516-27. DOI 10.1016/j.nurt.2008.08.002.
(56.) Gordon PH. Amyotrophic Lateral Sclerosis: An update for 2013 Clinical Features, Pathophysiology, Management and Therapeutic Trials. Aging Dis. 2013 Oct;4(5):295-310. DOI 10.14336/AD.2013.0400295.
(57.) Traynor BJ, Alexander M, Corr B, Frost E, Hardiman O. Effect of a multidisciplinary amyotrophic lateral sclerosis (ALS) clinic on ALS survival: a population based study, 1996-2000. J Neurol Neurosurg Psychiatry. 2003 Sep;74(9):1258-61.
(58.) Couratier P, Sindou P, Esclaire F, Louvel E, Hugon J. Neuroprotective effects of riluzole in ALS CSF toxicity. Neuroreport. 1994 Apr;5(8):1012-4.
(59.) Bensimon G, Lacomblez L, Meininger V. A controlled trial of riluzole in amyotrophic lateral sclerosis. ALS/Riluzole Study Group. N Engl J Med. 1994 Mar;330(9):585-91.
(60.) Miller RG, Mitchell JD, Moore DH. Riluzole for amyotrophic lateral sclerosis (ALS)/motor neuron disease (MND). Cochrane Database Syst Rev. 2012 Mar;3:CD001447. DOI 10.1002/14651858.CD001447.
(61.) Giess R, Naumann M, Werner E, Riemann R, Beck M, Puls I, et al. Injections of botulinum toxin A into the lateral sclerosis. J Neurol Neurosurg Psychiatry. 2000 Jul;69(1):121-3.
(62.) Pioro EP, Brooks BR, Cummings J, Schiffer R, Thisted RA, Wynn D, et al. Dextromethorphan plus ultra low-dose quinidine reduces pseudobulbar affect. Ann Neurol. 2010 Nov;68(5):693-702. DOI 10.1002/ana.22093.
(63.) Szczudlik A, Słowik A, Tomik B. [The effect of amitriptyline on the pathological crying and other pseudobulbar signs]. Neurol Neurochir Pol. 1995 Sep-Oct;29(5):663-74. Polish.
(64.) Drory VE, Goltsman E, Reznik JG, Mosek A, Korczyn AD. The value of muscle exercise in patients with amyotrophic lateral sclerosis. J Neurol Sci. 2001 Oct;191(1-2):133-7.
(65.) McClelland S 3rd, Bethoux FA, Boulis NM, Sutliff MH, Stough DK, Schwetz KM, et al. Intrathecal baclofen for spasticity-related pain in amyotrophic lateral sclerosis: efficacy and factors associated with pain relief. Muscle Nerve. 2008 Mar;37(3):396-8.
(66.) Marin B, Desport JC, Kajeu P, Jesus P, Nicolaud B, Nicol M, et al. Alteration of nutritional status at diagnosis is a prognostic factor for survival of amyotrophic lateral sclerosis patients. J Neurol Neurosurg Psychiatry. 2011 Jun;82(6):628-34. DOI 10.1136/jnnp.2010.211474.
(67.) Miller RG, Jackson CE, Kasarskis EJ, England JD, Forshew D, Johnston W, et al. Practice parameter update: the care of the patient with amyotrophic lateral sclerosis: multidisciplinary care, symptom management, and cognitive/behavioral impairment (an evidencebased review): report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology. 2009 Oct;73(15):1227-33. DOI 10.1212/WNL.0b013e3181bc01a4.
(68.) Chiò A, Logroscino G, Hardiman O, Swingler R, Mitchell D, Beghi E, et al. Prognostic factors in ALS: A critical review. Amyotroph Lateral Scler. 2009 Oct-Dec;10(5-6):310-23. DOI 10.3109/17482960802566824.
Publicado
Cómo citar
Número
Sección
Licencia
Derechos de autor 2016 Iatreia

Esta obra está bajo una licencia internacional Creative Commons Atribución-CompartirIgual 4.0.
Los artículos publicados en la revista están disponibles para ser utilizados bajo la licencia Creative Commons, específicamente son de Reconocimiento-NoComercial-CompartirIgual 4.0 Internacional.
Los trabajos enviados deben ser inéditos y suministrados exclusivamente a la Revista; se exige al autor que envía sus contribuciones presentar los formatos: presentación de artículo y responsabilidad de autoría completamente diligenciados.